Plus: Amphetamine and psychosis, and reimagining our approach to substance use prevention
By William Wagner
Issues centered on fentanyl continue to appear with frequency in this space—and it’s easy to see why. The synthetic opioid has emerged as a major driver of the overdose crisis. This week, we turn our attention to a valuable weapon in the fight against fentanyl-related deaths: test strips for the drug.
We also look at what amphetamines can do to the brain, and a new report on substance use prevention.
From HealthDay:
Testing for Fentanyl
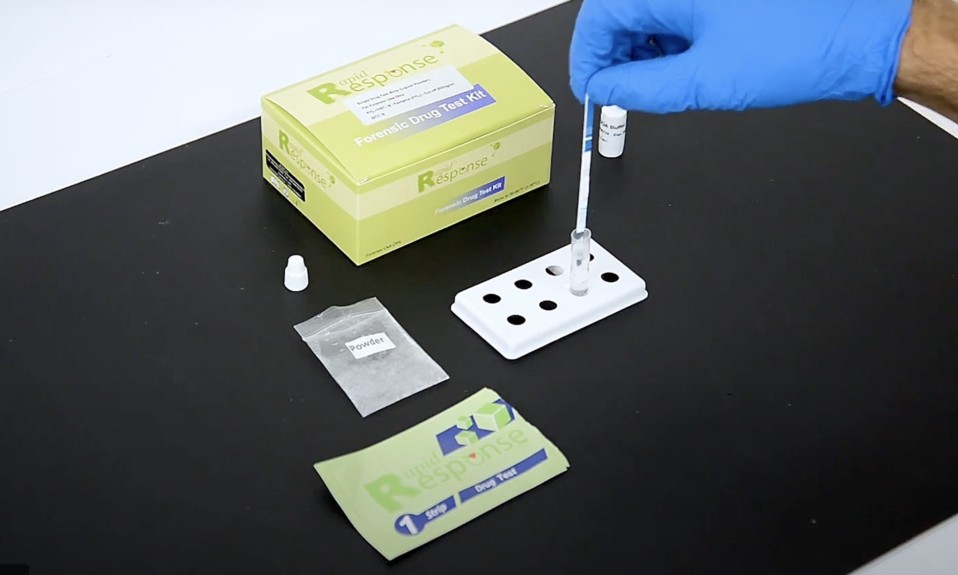
Fentanyl test strips won’t single-handedly solve the overdose crisis, but they can save a lot of lives—chiefly because so many other drugs are now adulterated with the extraordinarily potent synthetic opioid, from cocaine to MDMA. As Van Asher, a harm reduction coordinator with the nonprofit Housing Works, told HealthDay, “Fentanyl is now everywhere because people who sell substances do it to make money. Illicitly manufactured fentanyl is cheap. So, if I have a kilo of heroin and I add fentanyl, I can quickly turn it into several kilos for nothing.”
The strips, developed by the Canadian biotech company BTNX, are cheap (about a dollar apiece) and work quickly (they detect the presence of fentanyl in a drug within five minutes). For information on how to use fentanyl test strips, go to NYC.gov. Fentanyl test strips can be obtained from many syringe service programs (SSPs) and also from various harm reduction organizations.
From Evidence-Based Mental Health:
Amphetamine and Psychosis
Illicit amphetamine, a stimulant commonly called “speed,” can do irreparable damage to your brain, according to a newly published study in Evidence-Based Mental Health that was conducted by researchers from Taiwan. The study took place over 10 years and found that people who misuse amphetamine are up to five times more likely than the rest of the population to develop psychosis. Heavy use of the drug scrambles neurotransmitter signaling in the brain, triggering symptoms such as paranoia, voices in one’s head and hallucinations. In some cases, these psychotic episodes last for years.
“We … learnt that illicit amphetamine users who received rehabilitation treatment … were associated with a lower risk of psychosis.”
—study in Evidence-Based Mental Health
Interventions, the authors write, can improve outcomes: “We … learnt that illicit amphetamine users who received rehabilitation treatment … were associated with a lower risk of psychosis. This finding implies a preventive effect of psychotherapy for amphetamine use disorder on subsequent psychosis development. This is in line with previous findings on the efficacy of psychosocial interventions for cocaine and amphetamine use disorders.”
From the Partnership to End Addiction:
A Fresh Look at Substance Use Prevention

A comprehensive report by the Partnership to End Addiction calls for nothing less than a complete reimagining of strategies and policies aimed at substance use prevention. Titled “Rethinking Substance Use Prevention: An Earlier and Broader Approach,” the report argues that the focus on substance use prevention has been too narrow to make a substantial impact.
Meanwhile, the stakes couldn’t be higher for getting it right. “Youth substance use not only increases the risk of addiction but also has profound health, social, and financial costs,” the report reads.“It is directly linked to the three leading causes of death among adolescents—accidents, homicides, and suicide—and is implicated in poor academic performance, cognitive impairment, school dropout, unsafe sex, unintended pregnancies, mental health problems, violence, criminal involvement, unsafe driving, and numerous potentially fatal medical conditions. The more frequent and intense the use of addictive substances among young people, the greater the consequences.”
Among the suggestions in the report:
- Target the community and family rather than just the person using substances
- Initiate policies that break down the caregiving “silos,” such as by creating a federal coordinating body that is tasked with integrating resources
- Emphasize prevention education in schools, and provide that education earlier
- Become more data-minded in determining societal factors that lead to substance use
- Make racial equity a priority in substance use prevention funding
- Improve insurance reimbursement for healthcare services, such as by bolstering enforcement of the Mental Health Parity and Addiction Equity Act and other laws that prohibit discriminatory coverage for mental health issues and substance use disorder (SUD)
- Provide better SUD training in pediatric clinical settings
- Reduce the stigma surrounding SUD
- Expand research