Plus: An anti-stigma toolkit, and the very real danger of bicycling under the influence
By William Wagner
Heavy drinking is a threat to anyone, but women seem to be more vulnerable than men to its perils. A newly published study points to a significant rise in alcohol-involved suicide among women over the previous two decades.
Also this week, we take a look at a new toolkit designed to reduce stigma, and a study that examines the relationship between bicycle accidents and substance use disorder (SUD).
From Addiction:
The Link Between Intoxication and Suicide Among U.S. Women
In a study supported by the National Institute on Alcohol Abuse and Alcoholism (NIAAA), researchers discovered that women who are intoxicated are at “notably” greater risk for suicide than men. (Intoxication, or “alcohol-involved,” is defined as a blood alcohol concentration of 0.08 g/dL or greater.) Analyzing data from the National Violent Death Reporting System, the researchers found that the rates of alcohol-related suicides among women in all age groups measured (young adults, 18-34; middle-aged adults, 35-64; older adults, 65-plus) increased significantly every year of the study (2003-18). Among men, in contrast, the only significant year-over-year increases were in the middle-aged group.
“The researchers say these findings suggest that alcohol use may have been a core driver in the accelerated increase in suicide among U.S. women.”
—National Institute on Alcohol Abuse and Alcoholism
The study sheds at least some light on female suicidality in the U.S. Noting that non-alcohol-related suicide among women also increased during the course of the study, an NIAAA news release states: “The researchers say these findings suggest that alcohol use may have been a core driver in the accelerated increase in suicide among U.S. women. Although more research is needed to elucidate the link between alcohol use and suicide, the findings point to a need for more education and awareness of this relationship, as well as improved screening and intervention strategies.”
From the University of British Columbia and Western University:
A Toolkit to Combat Stigma
Stigma stands as one of the greatest obstacles to producing better addiction outcomes. The EQUIP Equity Action Kit, developed by the University of British Columbia and Western University in Canada, is meant to help healthcare providers and social service organizations address the persistence of addiction stigma.
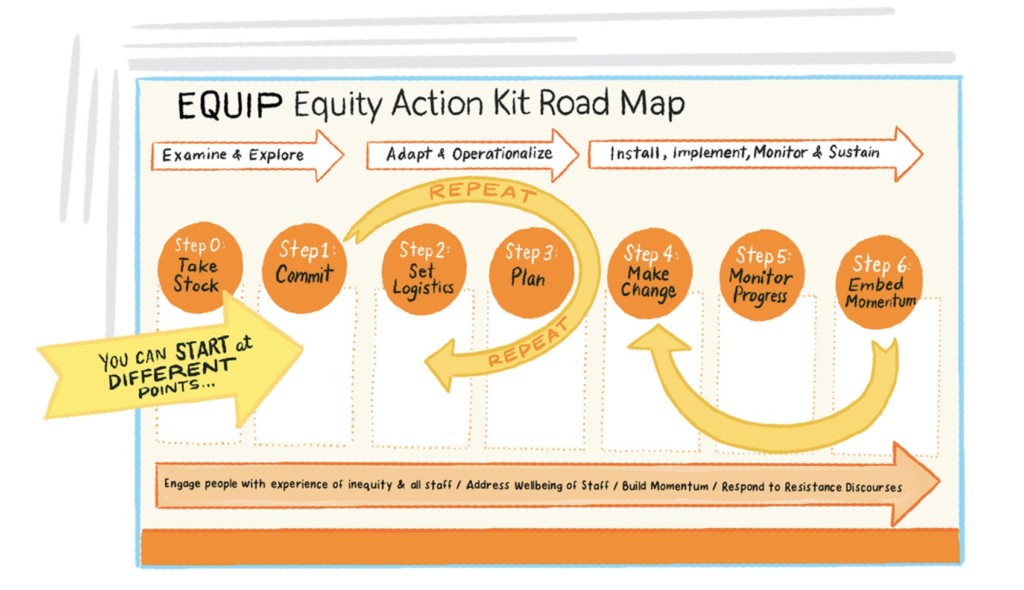
“We partnered with health and social service providers and people with lived experience to develop guidance, strategies and resources to improve pathways to care for people who experience substance use stigma and related types of discrimination,” says project co-lead Annette Browne, PhD, RN, a professor of nursing at UBC. “A key goal is to help organizations, staff and providers to deliver care that is non-judgmental, and that will encourage people to seek help when they need it—not avoid seeking help.”
Included in the toolkit:
- A step-by-step roadmap for reversing stigma
- A workbook for each step
- A suite of strategies and resources for implementation
- Guidance on how to overcome certain implementation barriers
- Guidance for estimating budgets and assessing success
The toolkit creators think it has the potential to bring about wholesale change. “The action kit supports engaging with people with experiences of stigma and poor care, meaning that their voices are always heard and prioritized,” says project co-lead Nadine Wathen, PhD, a professor at the Arthur Labatt Family School of Nursing at Western University. “These tools support large-scale implementation efforts to catalyze organizational and system change and improve health and social services and health outcomes.”
From the Journal of Studies on Alcohol and Drugs:
Bicycling Under the Influence

We all know drinking and driving is bad. Turns out drinking and bicycling is harmful as well. According to a new study in the Journal of Studies on Alcohol and Drugs, more than 11,000 people who had used drugs and/or alcohol were treated in ERs for bicycle-related injuries in 2019 and 2020. About 22% of the total incidents involved alcohol. The most common drugs detected in the systems of the patients were meth, marijuana and opioids.
Lead author Bart Hammig, PhD, MPH, of the University of Arkansas says those ER trips can serve as a tipoff, especially since a person’s presence on a bike might be related to SUD (homelessness, driver’s license revocation due to a DUI conviction). “When these patients present to the emergency department, it becomes important not only to treat the injuries but also to refer patients to drug treatment in an effort to intervene and prevent further negative events related to drug use,” he says.
Top photo: Zachary Kadolph













