As the state starts to allocate opioid settlement money, a debate is arising over the compatibility of spiritual approaches with medication-assisted treatment
By Mark Mravic
Across the country, states are beginning to receive money from opioid settlements with pharmaceutical manufacturers, drug distributors and pharmacies. In the coming months and years, more than $30 billion will be flowing through the pipeline to fund treatment, prevention, recovery, education and social outreach. Each state has established its own plan on how funds will be allocated—in most cases a split between the state itself and localities, and in some instances also a fund overseen by an advisory authority. Providers, advocates and other stakeholders eagerly await the influx of much-needed resources to build out treatment services and infrastructure and beat back the substance use epidemic.
But with all that money sloshing around, there will inevitably be competing interests at play, even when the objectives—reducing addiction, saving lives—are the same.
North Carolina’s Action Plan
North Carolina is a case in point. This spring and summer the state will get the first two installments—totaling some $93 million—of the $758 million it’s set to receive over the next 18 years. The state has long been anticipating how to allocate funds, releasing its initial plan in 2017 and updating it in 2019 and 2021.
The invaluable Opioid Settlement Tracker calls North Carolina’s information-sharing set-up “truly best-in-class” and a model that other states should emulate. It includes a wealth of resources for local policymakers, as well as dashboards with county- and city-specific data on opioid use, community drivers of health (poverty, uninsurance, unemployment, housing problems, incarceration, suicide), payment schedules for each locality in the state, and an action-plan dashboard to track progress and measure impact. The wealth of available information and guidance will be a boon to North Carolina patients, providers and those determining how to spend the funds.
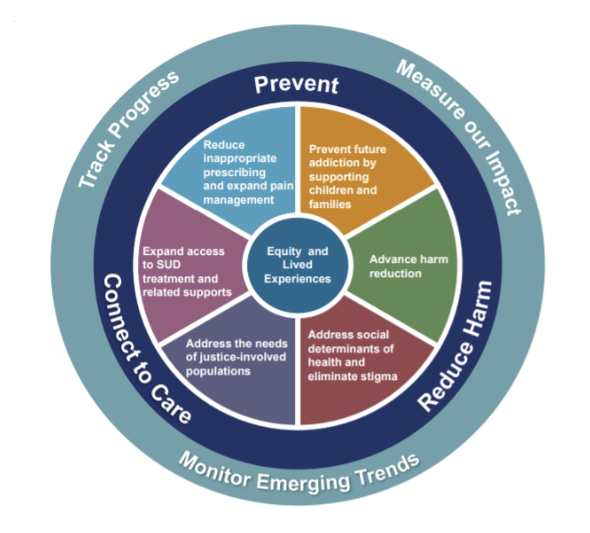
But that doesn’t mean the process will be friction-free. As reported by NC Health News, tensions are building between advocates who favor evidence-based treatment and groups offering a faith-based approach that in some cases can eschew harm reduction interventions such as medication-assisted treatment (MAT). And an aspect of the state’s allocation plan may be the root of such friction.
According to North Carolina’s Memorandum of Agreement, localities can choose either of two paths for allocating their funding.
Option A provides a short and specific list of “high-impact strategies,” centered on evidenced-based approaches and harm reduction, that local governments can support through existing or new programs. The strategies are:
- Collaborative strategic planning
- Evidence-based treatment, including MAT
- Recovery support services
- Recovery housing support
- Employment-related services
- Early intervention
- Naloxone distribution
- Post-overdose response teams
- Syringe service programs
- Criminal justice diversion programs
- Addiction treatment for incarcerated people
- Reentry programs for incarcerated people
Option B is more nebulous and open-ended, with emphasis on engaging “diverse stakeholders” and determining “shared vision” within communities. Evidence and harm-reduction are mentioned only in passing as approaches that may be considered, rather than as core strategies. Under Option B communities are encouraged to “identify goals” and develop process, quality and outcome measures. This more flexible (and vague) pathway, it seems, opens the door for a much wider range of programs and services, and “faith communities” are specifically identified in Option B as potential stakeholders for localities to consider when building out their plan.
Faith-Based Approaches
For instance, NC Health News points to a recently formed group called Bridge to 100, which plans to serve as a liaison between community leaders who control the opioid settlement purse strings and faith-based rehabilitation centers in each of North Carolina’s 100 counties. Among the providers Bridge to 100 says it’s working to assist are:
- Ground 40, an organization in Monroe, N.C., whose website says, “The heart behind our ministry is to facilitate this relationship with Christ that is portrayed in Psalms 40, and equip men with the biblical knowledge necessary to take on their daily lives in full confidence of who God is and who they are in Christ, while also providing them with the practical tools necessary to combat the temptations of this world with the strength of God, revelation of Jesus Christ, and help of the Holy Spirit.”
- Open Hands of Davidson County, whose mission is “to build relationships with our neighbors through help with physical needs, employment avenues and educational and spiritual activities which will ultimately lead to a relationship with Jesus Christ.”
- Adult & Teen Challenge, which provides “teens and adults freedom from addiction and other life-controlling issues through Christ-centered solutions.”
Faith has long played an integral and valuable role in addiction treatment. The 12-step program, which most faith-based treatment groups follow, has a storied history of effectiveness and millions of adherents. However, programs that follow the 12 steps often promote abstinence from all substances, including MAT—and sometimes can be seen as actively hostile to people taking medications such as methadone and buprenorphine, which are considered the gold standard for treating opioid use disorder.
Narcotics Anonymous (NA), for instance, notes that “within the context of NA and its meetings, we have generally accepted principles, and one is that NA is a program of complete abstinence. By definition, medically assisted therapy indicates that medication is being given to people to treat addiction. In NA, addiction is treated by abstinence and through application of the spiritual principles contained in the Twelve Steps of Narcotics Anonymous.” The organization notes that while anyone is welcome to attend meetings, those on MAT may be met by “members who express strong opinions about medically assisted treatment.” NA suggests that people should essentially shop around to find a group that may be open to MAT.
Similarly, while Bridge to 100 acknowledges the value of medication for short-term opioid detox, its site asserts that MAT “does not transform an addict’s life into one of freedom as a responsible, productive citizen of a community” and “does not provide long-term recovery.” To support those assertions, Bridge to 100 points to one study that found comparable six-month outcomes for subjects in a 12-step program who underwent medication-assisted treatment and those who did not.
But the authors of that particular study note that their main goal was actually to examine the feasibility of integrating MAT into a 12-step program (for which they found strong support), not to weigh long-term outcomes between MAT and abstinence. In fact, the authors specifically acknowledge that, based on how they conducted their study, “outcomes can be difficult to interpret. For example, it is possible that participants choosing medication treatment for opioid use disorder were different from those who did not in some meaningful way, and indeed they did appear to be experiencing more severe symptoms of opioid use disorder.” Moreover, rather than dismiss MAT’s importance after initial detox, the study’s authors emphasize the “additive benefits” of incorporating medication into a 12-step program.
The Importance of MAT
Meanwhile, a December opinion piece in the Charlotte Observer, by three addiction experts, took issue with the state’s funding of programs that eschewed MAT, including $10 million to a church ministry with no apparent previous addiction treatment experience. The authors of that editorial pointed to studies suggesting that rapid opioid detox followed by medication-free counseling—the kind of approach that some 12-step programs favor—fails in the majority of cases and “increases the risk of death.”
Addressing faith-based programs that perceive MAT to be incompatible with their spiritual mission, the authors of the Charlotte Observer opinion piece say, “That’s like asking a drowning person to choose between a lifejacket and prayer. There’s no reason you can’t have both.”
The hard fact, according to Kaiser Health News, is that fewer than half of North Carolina’s 62 long-term residential treatment facilities currently accept patients who take OUD medications, and just 12 are licensed to prescribe buprenorphine. That presents a serious problem for a state looking at how to spend hundreds of millions of dollars on effective opioid treatment.
Advocates for medication-assisted treatment don’t take issue per se with 12-step programs and other faith-based approaches. What MAT advocates, in North Carolina and elsewhere, puzzle over is why a spiritual, “whole person” approach to addiction treatment and recovery can’t also welcome proven medical therapies for what is acknowledged to be a chronic disease. Addressing faith-based programs that perceive MAT to be incompatible with their spiritual mission, the authors of the Charlotte Observer opinion piece say, “That’s like asking a drowning person to choose between a lifejacket and prayer. There’s no reason you can’t have both.”
The bottom line is to get the most effective forms of treatment to people who desperately need it. Ignoring or avoiding evidence-based approaches such as MAT will cost lives. Referring to the recent spike in overdoses from fentanyl, Raleigh, N.C., addiction provider Eric Morse told NC Health News, “Now the death rate is so high that if you’re not providing the best care at the very beginning, you’re letting people die. And in no other field of medicine would that be permitted.”